What is Clinical Integration?
Clinical integration can be defined in various ways depending on the circumstance. According to the American Hospital Association, clinical integration is defined as “necessary to facilitate the coordination of patient care across conditions, providers, settings, and time in order to achieve care that is safe, timely, effective, efficient, equitable and patient-focused. To achieve clinical integration we need to promote changes in provider culture, redesign payment methods and incentives, and modernize federal laws.”
Clinical integration plays a critical role in delivering patient data and meaningful insights to healthcare providers at the point of care. Physicians are currently working in “silos”, with critical healthcare data isolated within their walls. Many of these healthcare organizations lack the technical infrastructure and access to tools that allow them to securely send and exchange patient health information.
Recent government regulations and healthcare policy have significantly influenced the advancement of clinical integration over the past decade.
The Affordable Care Act (ACA) of 2011 included provisions to promote clinical integration and healthcare exchange between hospitals and health care organizations. Those policies promoted improved patient care coordination across the care continuum.
Most recent legislations include the Medicare Access and CHIP Reauthorization Act of 2015 (MACRA) which challenged health care organizations to collaborate in efforts to address concerns related to cost, quality and value. This further encouraged providers and healthcare organizations to invest in clinical integration to improve the coordination of patient care across the care continuum.
Why is clinical integration important?
As mentioned previously, many healthcare providers and organizations work with many disparate data sources and lack the ability to exchange pertinent patient health information with other healthcare organizations. The inability to exchange healthcare data with other providers prevents major risk
The purpose of integration in health care is to facilitate the coordination of patient care across the care continuum. Healthcare organizations need critical information on their patients and populations that are accurate, timely and actionable; to improve health outcomes and provide patient-focused healthcare.
These vital integrations help reduce overuse and improve the delivery of high value, high quality healthcare to patients. Without coordination across multiple organizations, patients are more likely to receive duplicative lab orders, diagnostic tests, have adverse prescription drug interactions and get conflicting care plans.
Clinical integration is a key component achieving the Institute for Healthcare Improvement’s “Triple Aim” of Healthcare initiative.
- To improve the patient care experience.
- To improve the health of populations.
- To reduce the cost of healthcare.
What is a Clinically Integrated Network (CIN)
According to Becker’s Hospital Review, a CIN “is commonly defined as a health network working together, using proven protocols and measures, to improve patient care, decrease cost and demonstrate value to the market”. In simpler terms, a CIN facilitates collaboration among health care providers.
In 1996, The Federal Trade Commission and Department of Justice defined it as “an active and ongoing program to evaluate and modify practice patterns by the CI network’s physician participants and create a high degree of interdependence and cooperation among the physicians to control costs and ensure quality.”
In its basic form, a CIN is a strategically aligned network of physicians, providers, organizations and offices that partner in efforts to provide quality care for patients in an efficient and cost-effective manner. To achieve success within a CIN, all stakeholders must be held accountable for their contributions to the system.
Performance benchmarks and standards must be met or adhered to for the group to be successful in a CIN. Physicians must be willing and able to participate in activities and initiatives that low healthcare cost, improve quality and the patient experience.
Examples of Clinical Integration
Here’s an example of an integrated care model:
- Large hospital systems integrated with regional Health Information Exchange to promote data sharing and to decentralize healthcare information to improve patient outcomes.
- Small Independent Primary Care providers integrating with local hospital systems in the area to receive alert when their patients are admitted to the hospital. Providers can use these alerts to reach out to their patients in a timely fashion to avoid further complications or readmissions to the hospital.
- Public Health Registries typically accept health information from healthcare organizations to promote behavioral health, vaccine, contagious disease surveillance and outbreaks.
Extract, Transform & Load (ETL)
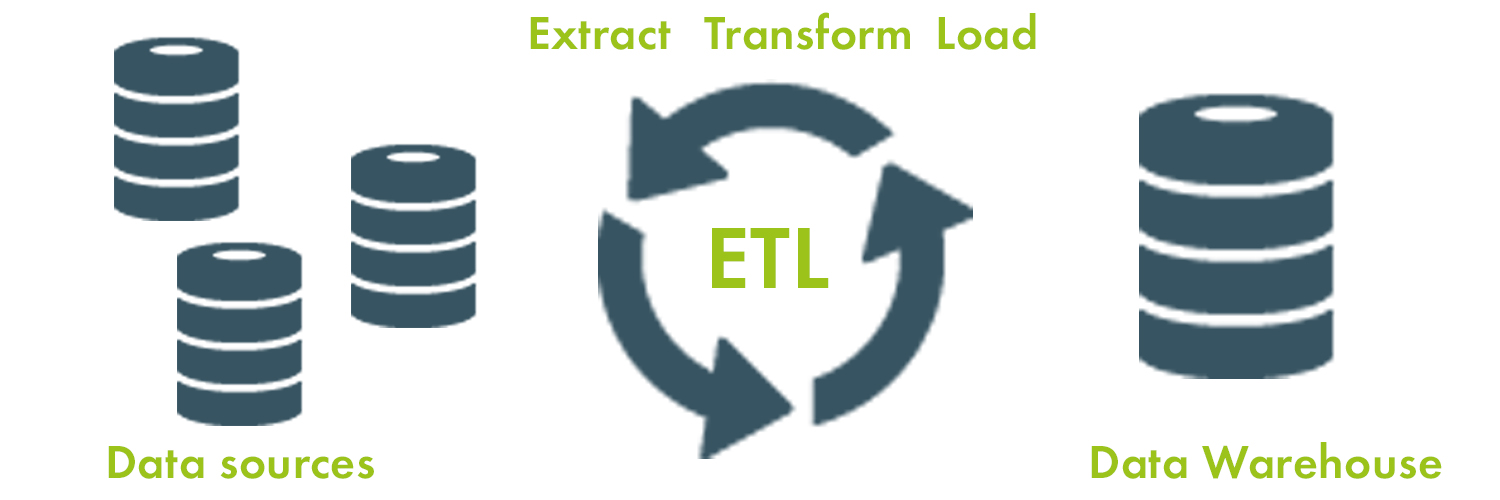
When discussing clinical integrations, there’s a common term that you may hear very often and that is ETL. Many people that are new to healthcare integration want to know what ETL is and what ETL stands for.
ETL also known as “Extract, Transform, & Load” refers to the processes required for copying data from one or more disparate sources into a destination system, database or data warehouse. The ETL process became popular in the 1970s and is often used in data warehousing and provides a foundation for clinical integrations and analyzing healthcare data.
ETL involves three steps.
- Extracting data data from various data sources;
- Transforming data by cleaning and transforming them into a standardized format for querying and analysis
- Load data into a database, data store, a data mart, data lake or a data warehouse.
These processes are completed by an ETL developer, but what is a ETL developer?
An ETL developer is a type of software engineer that uses ETL tools and software to manage data throughout the ETL pipeline. This role varies by title but typically includes roles such as Clinical Integration Specialist and Integration Architects.
There are many ETL jobs available to people skilled in databases, healthcare data standard and ETL packages, triggers, stored procedures, views, and SQL transactions.
Clinical Integration Standards:
Every ETL Engineer and developer must be familiar with healthcare data standards. These standards are considered the holy grail of clinical integration and sharing healthcare data.
Healthcare data standards serve a critical role in the coordination of patient care and how clinical integration is to be facilitated. Standards and guidelines help guide healthcare organizations on how to securely exchange healthcare data and the standards needed to implement systems to exchange healthcare data.
What is HL7 in healthcare
Health Level Seven or HL7 refers to a set of international standards for the transfer of clinical and administrative data between software applications used by various healthcare providers. HL7 specifies a number of flexible standards, guidelines, and methodologies by which various healthcare systems can communicate with each other.
These data standards and guidelines are a set of rules that allow information to be shared and processed in a uniform and consistent manner and allow healthcare organizations to easily share clinical information.
Over the past few years, HL7 has focused on its Fast Healthcare Interoperability Resources (FHIR) – a standard for the exchange of resources. But questions still arise regarding what is HL7 FHIR? Essentially, It allows healthcare information, including clinical and administrative data, to be available securely to those who have a need to access it, and to those who have the right to do so for the benefit of a patient receiving care.
FHIR was designed for easy implementation and helps leverage modern web-based suite of API technology, including a HTTP-based RESTful protocol, HTML and Cascading Style Sheets for user interface integration, a choice of JSON or XML for data representation, OAuth for authorization and ATOM for query results.
FHIR significantly lowers the barriers of entry for new software developers to support healthcare needs.
Roles in Clinical Integration
Data Integration and ETL engineers are responsible for facilitating the acquisition of healthcare data from external vendors to extract, transmit and load data into a data warehouse for data analysis.
At the core, the Data Integration Engineer focuses on extracting information from various internal and external sources, reviewing the data collected to transform and parse the data to make it usable, and finally, loading that data to a database to be analyzed later.
Engineers work closely with Project Managers and Implementation Specialists to develop ETL pipelines from external data sources to store, analyze and provide meaningful insights to providers at the point of care.
Clinical Integration roles involve:
- Troubleshooting and debugging clinical application systems.
- Checking incoming data for quality assurance, responding to data integrity issues and taking corrective measures.
- Developing and supporting interfaces to provide accurate and timely data for connected practices and other healthcare organizations.
- Collaborate closely with users and trading partners to design, develop, test, and monitor EDI communications.
- Create and manage ETL packages, triggers, stored procedures, views, and SQL transactions.
- Develop new secure data feeds with external parties as well as internal applications including the data warehouse and business intelligence applications.
- Perform regular analysis and QA, diagnose ETL and database related issues, perform root cause analysis, and recommend corrective actions to management.
- Work with a small project team to support the design, development, implementation, monitoring, and maintenance of new ETL programs.
7 Top Clinical Integration and ETL Developer Jobs
- Data Integration Engineer
- Clinical Integration Specialist
- HL7 Integration Engineer
- FHIR Integration Engineer
- Integration Architect
- Data Integration Data Analyst
- Medical Claims Integration Engineer
Skills Needed for Clinical Integration Roles
ETL job seekers will need some experience in a healthcare setting, especially regarding the flow of clinical data within an acute care hospital environment. They’ll need to understand Health IT standards and protocols, clinical data standards such as HL7 and FHIR, and be knowledgeable of Health Information Exchanges (HIE).
Having experience with programming languages such SQL, python, C#, and Java will increase the chances of you landing a role as a ETL developer.
Career seekers will need to know how to handle file types such as XML, JSON, and CSV files because these are typically used for transmitting healthcare data. It is most important that people in these roles understand ETL tools and software such as NextGen Connect/Mirth, Pentaho, and Iguana Integration engine.





Recent Comments